One of the least hailed impacts of the pandemic has been the explosive growth in Medicaid enrollment, which has increased by 10 million since February 2020. Medicaid and the Children’s Health Insurance Program (CHIP) now provide health insurance to 80.5 million Americans, which is more than Medicare and the VA combined.
With the largest enrollment in its more than 50-year history, Medicaid has become a fixture of the social safety net and a key part of American health care, covering a quarter of the US population, including 38.3 million children. In the shadow of calls for Medicare for All and a public option under Medicare, Medicaid has emerged as the health insurer many Americans are turning to for coverage.
“Medicaid and CHIP serve as a much-needed lifeline for millions of people throughout this country. The increase we are seeing is exactly how Medicaid works: the program steps in to support people and their families when times are tough,” said CMS Administrator Chiquita Brooks-LaSure. “For the parents that may have lost a job or had another life change during the pandemic, having access to coverage for themselves and their kids is life-changing. CMS is committed to ensuring our nation’s marginalized communities and low-income families have the coverage they need.”
Medicaid enrollment in Oregon from March 2020 to December 2020 grew by almost 15 percent. In the same period Washington’s enrollment rose more than 11 percent. Nevada registered the largest percentage growth at 32 percent, followed by Missouri, Indiana, Wisconsin, Nebraska and Florida.
Prior to the start of the pandemic, Medicaid enrollment growth nationally was flat and there was substantial enrollment churn. During the pandemic, a special enrollment period was created that lasted through August 2020. Eligibility checks were halted, and states were prevented from dropping Medicaid enrollees.
Medicaid and Medicare were created in the 1960s as part of President Lyndon Johnson’s War on Poverty. Medicare drew the biggest headlines by providing universal health insurance coverage for older adults. Medicaid received less attention for offering a health insurance lifeline to lower-income families, pregnant mothers and disabled Americans.
While Medicare is paid for entirely by the federal government, Medicaid costs are shared by the federal government and individual states, which has set up budget battles in state legislatures and led to various forms of provider taxes. The federal government pays the largest share of Medicaid and sets basic coverage standards. States have authority and latitude to set the rules to qualify for and retain coverage.
The Affordable Care Act created an option for states to expand Medicaid coverage to uninsured individuals and families with incomes exceeding the poverty line by up to 138 percent, which translates into an annual income of $17,774 for an individual, $23,169 for a two-person household and $35,245 for a family of four. For reference, a person working full-time and paid at the federal minimum wage of $7.25 per hour earns $15,080 annually. A full-time worker paid at $11 per hour earns $22,880.
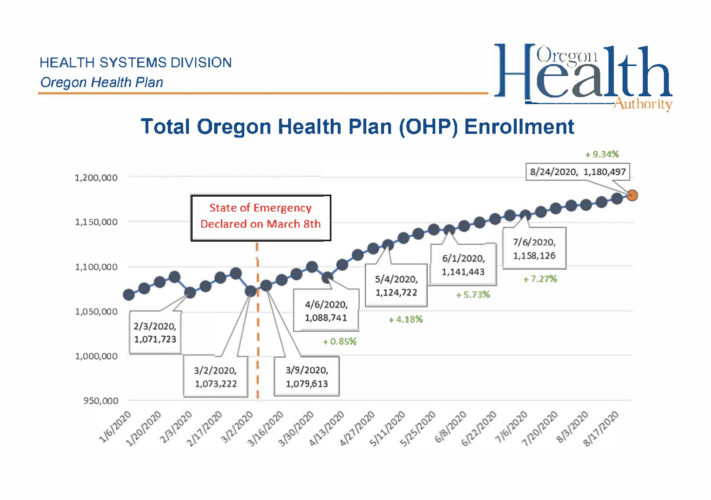
Oregon and Washington were among the states to accept the Medicaid expansion invitation. Oregon has tied its Medicaid system, called the Oregon Health Plan, to innovations such as Coordinated Care Organizations and in-home care, which were designed to improve the quality, delivery and efficiency of healthcare services to Medicaid populations.
A dozen states, including Texas and Florida, have declined to expand Medicaid eligibility, which health experts say could swell Medicaid enrollment by another 30 million. The American Rescue Plan contained lucrative incentives to expand their state Medicaid plans, though so far that hasn’t convinced states, which are mostly in the south, to rethink their decision.
During the Trump presidency, states were allowed to impose work requirements on some Medicaid recipients, even though 25 percent of enrollees are over age 65 or disabled and 12 percent are already working full-time or part-time. President Biden has withdrawn that permission. Critics claim Trump administration officials made it harder to enroll, which contributed to sluggish growth in Medicaid enrollment and a 1 million decline in coverage of children between December 2017 and June 2019.
Previous Medicaid enrollment spurts have occurred during economic downturns, though mostly involving coverage for children. During the pandemic, Medicaid enrollment growth centered on adults. Enrollment growth during the pandemic has been more intense than in the previous recession in 2009 when fewer than 4 million Americans newly enrolled in Medicaid.
With the latest Supreme Court challenge to the Affordable Care Act swatted away, expanded Medicaid eligibility seems secure. With congressional gridlock, major changes to the Affordable Care Act or a more comprehensive replacement seem politically unlikely. That may lead to greater focus on improving and further expanding Medicaid.
There has been talk of integrating care for the more than 11 million older adults and disabled persons who are eligible for coverage under both Medicare and Medicaid. More than half of dual eligible beneficiaries suffer from three or more chronic disease. Their care consumes 34 percent of total Medicare costs and 33 percent of total Medicaid costs, and yet 90 percent receive fragmented care, ranging from overlooked symptoms to misdiagnosed illnesses. Based on 2015 data, 56 percent of nursing home patients in Oregon were covered by Medicaid. In Washington, it was 59 percent.
Some futurists predict the overall healthcare system, including Medicaid, will swivel from treating disease to preventing it. There is hope diabetes and cancer, like polio, could be eradicated or significantly reduced by medical advances and improved preventive care.
The increase we are seeing is exactly how Medicaid works: the program steps in to support people and their families when times are tough. For parents that have lost a job or had another life change during the pandemic, access to coverage for themselves and their kids is life changing.
Since Medicaid covers some of America’s most vulnerable people, it will need fulsome wellness programs and tools. One idea is to arm Medicaid participants will smart medical devices for home and personal use to improve disease detection, enable routine monitoring of chronic diseases and promote healthy practices. Smart medical devices, which could be as simple as apps or a virtual assistant, would be a covered Medicaid benefit, giving health care providers routine and timely access to data that can inform care, such as when a test, office visit or medication change is required.
Smart devices could enable formation of virtual groups for patients with similar conditions, expanded use of telemedicine and wellness organizations that pool resources and best practices to serve Medicaid populations. With a stronger focus on preventive care, Medicaid could integrate health care providers with social workers and mental health professionals.
Deloitte Insights published a thoughtful article titled “Medicaid in 2040” that lays out a potential future for the program. Here is an excerpt about how a Medicaid patient might benefit from a smart medical device:
Racquel is a 32-year-old Medicaid beneficiary who is on maternity leave from her job and home alone with her newborn most of the day. She feels overwhelmed and isolated and has been diagnosed with postpartum depression.
Like most people, Racquel has a virtual assistant at home, which she uses for everything from inquiring about the weather to ordering groceries for delivery. Her virtual assistant also can detect changes in her mood, based on the sound and pitch of her voice.
Today, the virtual assistant has detected an alarming change in her mood, and alerts Racquel’s mental health provider. The mental health provider reaches out to schedule an emergency video consultation to assess whether Racquel requires in-person assistance or whether her medications need to be adjusted. The 20-minute consultation confirms that Raquel is okay and offers support and mental health strategies, encouraging her to leave the house and attend the local New Moms group with her baby.
The New Moms group, which meets at a local library, is an extension of the virtual group by the same name. It is a smart health community in which new mothers share useful tips about a range of topics, including managing postpartum depression. Data about Racquel’s mood, which is assessed and collected by her virtual assistant, demonstrates that her mood improves when she participates in the group, either online or in person.
The virtual assistant often “nudges” Racquel to log into the group’s console when her mood dips below a certain threshold, and it will encourage Racquel to attend an in-person meeting if one is being held that day within five miles of her home.